Few elective medical procedures generate as much curiosity — and as much cautious hesitation — as LASIK. The idea of permanently correcting your vision without glasses or contacts is genuinely appealing, and for millions of people who have undergone the procedure, it has delivered exactly that. But curiosity and hesitation tend to travel together when the thing being discussed is a laser pointed at your eye. People want specifics: what the surgery involves step by step, whether it hurts, how quickly vision improves, and what the realistic risks look like.
The good news is that LASIK has a well-documented track record spanning more than two decades of widespread clinical use. It is not an experimental procedure or a recent innovation — it is a mature surgical technique with refined protocols, predictable outcomes in appropriately selected patients, and a post-operative experience that most people describe as far more manageable than they anticipated. Understanding what that experience actually looks like, rather than relying on secondhand anxiety or outdated assumptions, is the most useful thing a prospective patient can do before walking into a consultation.
The Mechanics Behind the Procedure
LASIK — laser-assisted in situ keratomileusis — works by reshaping the cornea, the clear front surface of the eye that plays the primary role in focusing incoming light. In a healthy eye without refractive error, light focuses precisely on the retina, producing a sharp image. In a myopic eye, the cornea is too steeply curved, causing light to converge short of the retina. Hyperopia involves the opposite problem: insufficient curvature that pushes the focal point behind the retina. Astigmatism results from an irregular corneal shape that scatters focus across multiple points. LASIK corrects all three by using a precisely calibrated excimer laser to remove microscopic amounts of corneal tissue and alter its curvature.
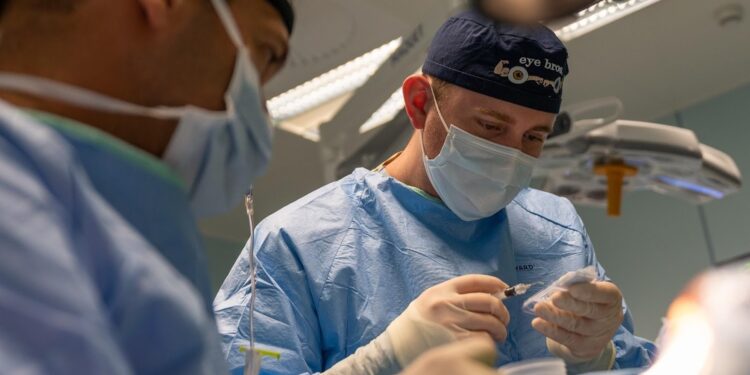
Before the laser can be applied, the surgeon creates a thin flap in the outer corneal layer — the epithelium and part of the stroma — using either a mechanical microkeratome or, more commonly in modern practice, a femtosecond laser. The flap is folded back to expose the underlying stromal tissue, the laser delivers its treatment over a matter of seconds, and the flap is then repositioned. No sutures are needed; the flap adheres naturally through the eye’s own healing process. The entire bilateral procedure — both eyes — typically takes under thirty minutes, though the active laser time per eye is often fifteen to sixty seconds depending on the prescription being corrected.
How Candidacy Is Evaluated
Not everyone who wants LASIK is an appropriate candidate, and the pre-surgical evaluation is designed specifically to identify who will benefit and who would be better served by an alternative approach. Corneal thickness is among the most critical measurements — the procedure removes tissue, so there must be sufficient depth to reshape the cornea safely while preserving the structural integrity of what remains. Patients with thin corneas may be redirected toward surface ablation procedures like PRK, which do not require flap creation, or lens-based corrections for higher prescriptions.
Prescription stability is another prerequisite. Surgeons generally look for at least one to two years of stable refraction before proceeding, because operating on a prescription that is still shifting will produce results that change over time. Dry eye disease, keratoconus, and certain autoimmune conditions can also disqualify candidates or require additional evaluation before a decision is made. The consultation process is thorough for a reason — the outcomes data supporting LASIK’s efficacy is drawn from patients who were properly selected, and the results in that population are substantially better than in patients for whom the procedure was not optimally indicated.
What Happens in the Days and Weeks After Surgery
The immediate aftermath of LASIK tends to surprise patients in a positive direction. Most people notice meaningful visual improvement within hours of the procedure, and a significant number are seeing clearly enough to drive the following day. The first few hours post-operatively are typically characterized by a watery, gritty sensation and light sensitivity, which generally resolves as the initial healing phase progresses. Surgeons typically advise patients to go home and sleep for a few hours after surgery, which both accelerates early healing and bypasses the most uncomfortable portion of the immediate post-op window.
The recovery trajectory from that point forward varies somewhat between patients, but the broad contours are consistent. Vision at day one is often surprisingly good but may fluctuate over the following weeks as the corneal epithelium continues to heal and the brain adapts to processing a fundamentally different visual signal. Halos, starbursts around lights, and mild glare — particularly noticeable at night — are common during the first month and diminish for most patients as the eye stabilizes. For a detailed week-by-week breakdown of what to expect through the full healing process, this guide to how long recovery after LASIK takes is one of the more thorough resources available for patients preparing for the post-operative period.
Activity Restrictions and Protective Measures
Recovery restrictions after LASIK are less burdensome than many patients expect, though they do require some adjustment to routine. Swimming and hot tubs are off-limits for several weeks to protect against infection while the flap interface heals. Contact sports that risk eye impact require protective eyewear or temporary avoidance. Rubbing the eyes — a common reflex response to dryness or irritation — is strongly discouraged during the healing period because pressure on the eye can disturb the flap before it has fully adhered. Eye drops play a central role in recovery: antibiotic drops to prevent infection, steroid drops to manage inflammation, and preservative-free artificial tears to combat the dryness that is one of the most frequently reported post-operative side effects.
Most patients return to office work and screen-based tasks within a day or two, though extended screen time may feel fatiguing for the first week. Outdoor activity is generally permitted quickly, with the practical caveat that sunglasses should be worn to protect the healing cornea from UV exposure and wind. The post-operative schedule typically includes visits at one day, one week, and one month, with additional follow-ups if the surgeon identifies anything requiring closer monitoring.
Informed Decision-Making and Finding the Right Resources
One of the more consistent patterns in how patients approach elective eye surgery is that those who invest time in understanding the procedure before their consultation tend to have a better experience overall. They ask more targeted questions, process the surgeon’s recommendations more confidently, and manage their recovery expectations more accurately. The anxiety that surrounds LASIK for many prospective patients is often inversely proportional to how much they actually know about what the surgery involves — the less specific their understanding, the more room there is for worst-case thinking to fill the gaps.
Quality information sources matter in this context. Academic medical centers with dedicated ophthalmology programs — such as the ophthalmology department at Massachusetts General Hospital — publish patient education resources that reflect the standards of care practiced in high-volume, research-active clinical environments, and consulting these alongside your surgeon’s own materials provides useful calibration. For broader coverage of the surgical options available across the spectrum of vision correction, Eye Surgery Today offers procedure-specific content that is accessible to patients without a clinical background while remaining medically grounded enough to genuinely inform the decision-making process.
Weighing the Long-Term Picture
LASIK results are durable for most patients, but durability is not the same as permanence in every case. The corneal reshaping itself is permanent — the tissue removed does not regenerate. However, the eye continues to change with age. Presbyopia, the age-related loss of near-focus flexibility that affects virtually everyone in their mid-forties, will develop regardless of whether a person has had LASIK. Patients who have LASIK in their twenties or thirties will very likely need reading glasses eventually, just as their non-LASIK peers will. For a small percentage of patients, a secondary enhancement procedure may be recommended years later if the prescription shifts meaningfully over time.
The informed way to approach LASIK is not as a one-time fix that eliminates all future vision considerations, but as a highly effective intervention that — for the right candidates — delivers years or decades of freedom from distance correction while understanding that the eye continues to age normally. Framed that way, the value proposition is clear and the expectations are realistic. Patients who understand this going in tend to remain satisfied with their outcomes far more consistently than those who expected permanent, total freedom from any vision correction for the rest of their lives.
The procedural landscape for vision correction has never been more refined, and the information available to help patients navigate it has expanded considerably. What determines whether someone benefits from that landscape is largely whether they engage with it carefully — starting with honest self-assessment, moving through a rigorous candidacy evaluation, and following through with diligent post-operative care. That combination, more than any individual factor, is what separates excellent outcomes from disappointing ones.


 Home
Home