The history of patient care is a story of constant evolution, one that has shifted dramatically from personalized, at-home attention to technology-driven hospital treatments. Now, it’s turning back again to focus on individual care within the comforts of home. This transition from the clinical to the personal touches at the heart of healthcare’s most fundamental goal: to provide care that is not only effective but also comforting and convenient.
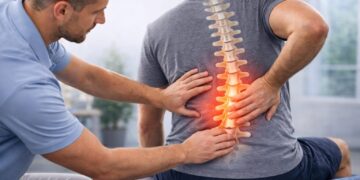
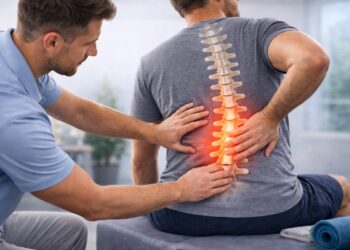
In today’s fast-paced world, the concept of medical practitioners visiting patients at home is gaining popularity, as it offers a level of comfort and individual attention that hospitals are often too busy to provide. Medical house calls, which once seemed on the brink of obsolescence, are now being recognized as an innovative solution for certain patient groups. These calls represent a bridge between the personalized care of the past and the sophisticated, tech-infused healthcare of today. This article will delve into how this traditional method of care is being reimagined to fit into our current healthcare landscape.
Table of Contents
1. The Resurgence of Medical House Calls
The practice of doctors visiting patients at home, known as medical house calls, has been gaining popularity, transforming into a system where technology enhances rather than replaces the human touch. Historically, home visits were a common practice, but they dwindled with the rise of large hospitals equipped with advanced medical technologies. Now, they’re making a surprising return.
Modern medical house calls signify a shift towards more patient-centric care, where services are not limited to a hospital or clinic. Patients with mobility issues, chronic conditions, or those requiring palliative care can receive comprehensive medical attention in their own homes. The variety of services that can be delivered directly to a patient’s home now includes routine follow-ups, complex chronic disease management, acute illness treatment, and even some emergency interventions.
This re-emergence of house calls has been made possible through several factors. On one side, there’s a growing preference for the comfort and familiarity of home during recovery or treatment. On the other, advancements in medical technology have played a crucial role. Portable medical devices and improved communication tools now allow healthcare providers to offer an array of services that were once only possible in a hospital setting.
2. Technological Advancements Enabling Home Care
The integration of technology into home care has revolutionized what it means to receive medical services. Telemedicine has emerged as a critical component, making it possible for patients to have virtual visits with healthcare providers through video conferencing. This development has not only made healthcare more accessible but has also made it possible to offer continuous care, essential for patients with chronic illnesses or those in need of post-operative care.
Furthermore, mobile health applications and wearable devices provide real-time health data to practitioners, allowing for constant health monitoring. The use of these devices means patients no longer need to be in a hospital to receive constant care. Innovations such as wearable heart monitors and blood glucose testing kits enable doctors to keep track of their patient’s health with minimal intrusion into their daily lives.
Portable diagnostic tools have also enhanced the capability of healthcare professionals to bring hospital-level diagnostic services to the patient’s home.One notable tool in this regard is the RightSpotpH® Indicators, which can be used both in hospitals and homes. These indicators verify gastric acidity levels to ensure the correct placement of NG/OG tubes.
Furthermore, innovations in technology have enabled ultrasounds, ECGs, and X-rays to be conducted beyond the confines of traditional clinical settings. This means that comprehensive medical care can now be delivered at home, benefiting a wider range of individuals.
3. The Role of Home Healthcare Services
Home healthcare services encompass a broad range of care procedures that one can receive in the comfort of their own living space. These services can be as simple as helping with daily activities for older adults or as complex as nursing care for patients with chronic illnesses. The scope is wide, including physical therapy, occupational therapy, speech therapy, and even social work.
The teams responsible for providing home healthcare include a diverse group of healthcare professionals. Registered nurses, physical therapists, occupational therapists, home health aides, and social workers can all be part of a home care team. They work in coordination to ensure that a patient’s recovery or maintenance plan is executed effectively, mirroring the multidisciplinary approach of hospitals.
One of the most critical aspects of home healthcare is the continuity of care. When a patient moves from the hospital to their home, the transition needs to be smooth to prevent any lapse in treatment. Home healthcare services ensure that the same level of care continues, minimizing the risk of complications or readmissions to the hospital. Studies and real-life success stories underscore how well-managed home healthcare can lead to faster recovery times, improved health outcomes, and enhanced quality of life.
4. Economic Implications
The economic benefits of shifting patient care from hospitals to homes can be substantial. Hospital stays are expensive, not just for the patient and their families but also for the healthcare system as a whole. Home care can significantly reduce these costs by shortening or eliminating the need for hospital stays. When care is provided at home, the expenses related to hospital infrastructure, in-patient services, and staffing are reduced.
For many, the question of how health insurance fits into home healthcare is of significant concern. Today, more insurance companies are recognizing the value of home-based care and are beginning to cover these services under their plans. This shift is a reflection of the cost-effectiveness and the growing demand for home care options.
Economically, when home care becomes part of the broader healthcare system, it has the potential to save billions of dollars. By preventing hospital readmissions and reducing the length of hospital stays, home care can lighten the financial load on healthcare systems, making resources available for other critical areas.
5. Challenges and Limitations
Despite its many advantages, the move towards home-based care isn’t without its challenges. There are barriers to the widespread adoption of this model, including a shortage of healthcare professionals trained in-home care and the geographical limitations of reaching remote or underserved populations.
Quality control and safety are also paramount concerns. Ensuring that home healthcare providers maintain high standards of hospital care requires robust oversight and regulation. Additionally, adapting the regulations to accommodate the unique aspects of home healthcare, including privacy concerns and the safety of healthcare workers, is an ongoing challenge.
Nevertheless, overcoming these challenges is not insurmountable. With focused policy-making, investment in training, and technological innovation, the future of home-based care looks promising. It’s about creating a sustainable model that can support the growing need for in-home care services, particularly as populations age and the demand for such services increases.
Conclusion
The evolution of patient care from the hospital to home reflects a healthcare system in flux, striving to meet the changing needs of society. This journey back to the roots of personalized care, now equipped with modern technology and new insights, is paving the way for a future where home is not only where the heart is but where healing happens, too.


 Home
Home